Why Syria’s health service needs foundational support
Published: Jan 27, 2021 Reading time: 5 minutes Share: Share an articleOnce a country with a talented pool of doctors and health care workers, Syria now finds itself emptied of professions. Migration in search for better opportunities abroad began some decades back but for the past 10 years, they are looking for refugee status fleeing an atrocious war.
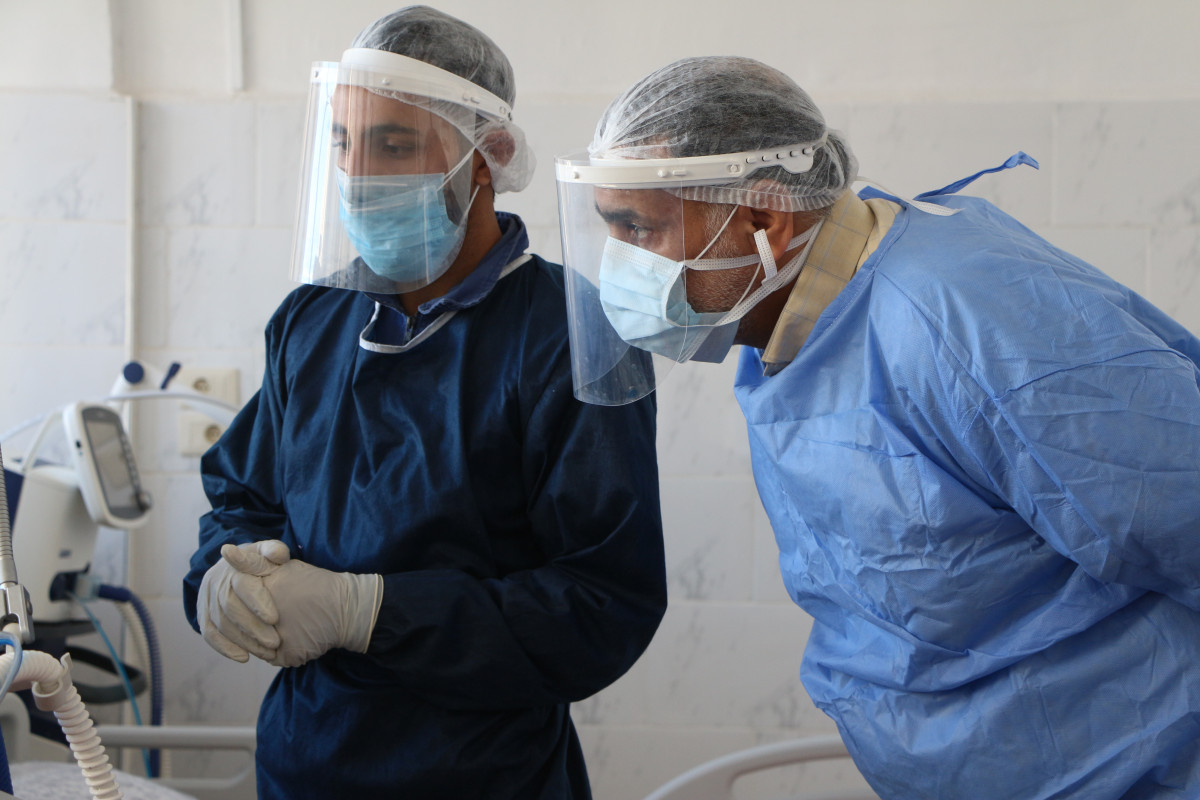
The remaining medical staff in the country are facing unprecedented challenges, one after another. Health facilities have been targeted by different parties in the conflict violating the International Humanitarian Law, also known as the rules of war, which consider attacking civilians or civilian infrastructure illegal.
Earlier this year, the World Health Organisation considered that “of all armed conflicts across the globe, Syria has for years been one of the worst examples of violence affecting health care” from intentional attacks on sites where the sick and wounded are treated, to restricting or denying civilian access to health care.
The COVID-19 pandemic now puts these frontline workers at an even greater risk, with a lack of personal protective equipment (PPE), medical equipment, facilities and capacities. They are striving to treat those acute cases, while risking their own health in the process. In such conditions, it’s hardly impossible to avoid the stereotype lauding the health workers who remain in Syria as heroes.
“Above all, I am a doctor, a Syrian physician. Regardless of anything, I provide humanitarian service at all times and my motivation is a humanitarian one,” says Dr. Muhammad*, who has been practising medicine continuously and resisting all kinds of security and political situations to do so. “The armed conflict made life very difficult, but the emergence of COVID-19 made lives even worse”.
Some areas** like where Dr. Muhammad works are particularly vulnerable because they are at the crossroads of different regions hosting large displaced populations. His health centre is trying to provide public health for a population of 350,000 living in this district, but also to many other people outside the district who have nowhere else to go, as a medical assistant of the new intensive care unit in a public hospital, Ahmed, reports.
Since the entire region did not have almost a single ICU of their own, the hospital had not many options up until this point. Facilities had been neglected due to lack of funding or proper management and support from all governance levels. “We had no choice but to receive COVID-19 patients along with other patients, with the risks that implied," nurse Fatima regrets.
Furthermore, a great deal of medical supplies arrive to Syria through UN cross-border and cross-line aid, which lately is finding additional obstacles due to the non-renewal of cross-border crossing points by the UN Security Council.
The onslaught of the pandemic thwarted an initial PIN project that focused on institutional repairs. Instead, PIN accelerated a more urgent emergency response working in cooperation with an international NGO health partner and a local health provider: After the completion of an assessment of existing hospitals, PIN began identifying contractors to undertake the repairs needed to ensure that health facilities had adequate space for potential patients by refitting whole units into isolation mode or by building new ones. With funds from the USAID’s Bureau for Humanitarian Assistance (BHA), activities in 3 hospitals accounted for 1,548 square metres to host 46 beds in intensive care units and 21 beds in a moderate-case unit.
“Due to the extreme scarcity of intensive care beds, we focused our efforts on setting up intensive care/isolation units in different governorates. Thanks to a successful and well-coordinated joint effort between donor and partners, we were able to identify the locations, design, approve and build 3 intensive care units and 1 moderate cases unit in 3 different governorates in northern Syria a period of only 4 months,” PIN Shelter advisor in Syria explains.
Ali is a 30-year-old with two children that recovered from COVID-19 after being admitted in one of the intensive care units designed by PIN. After this “scary” experience he admits to be now advising everyone to adhere to preventative measures. While in the hospital, he explains he felt comforted by the medical staff, which was important for him to be in good spirits to go back to his family healthy. “I kept telling to myself that once I recovered, I would talk to people about my experience with COVID-19 to make them be more careful, and protect everyone’s health by following the guidelines to prevent spreading the disease.”
“War has destroyed the infrastructure in the region in general and medical [infrastructure] in particular. And given our modest capabilities, we should be focusing a lot on prevention,” explains the administrative director of the hospital. Dr. Muhammad agrees: “The individual who is infected is convinced of COVID-19 being real and dangerous and not an invention shared on social media, but someone that sees it from afar doesn’t realise what is going on.”
However, authorities, aid and health stakeholders are struggling to raise awareness around how crucial preventative measures such as social distancing, masks, hygiene are. Yet when people are struggling to buy food, how can they think of a more abstract danger like COVID-19?
“I think that recovered persons with influence in the community (like tribal sheikhs and administration officials) should talk about their fight against the disease,” the unit Doctor thinks that would be effective to spread awareness. “As it is said: An ounce of prevention is better than a pound of cure.”
Despite all, this doctor will continue to work no matter the circumstances, as he always has. “Our needs are many: We have just a few respirators so far. Now it's okay. But when the number of patients double, like statistics predict will be the case, we will need about 20 to 30 additional respirators.”
*Names of people have been changed in the article for security reasons
**PIN is vague about specific locations of our activities to preserve safety and security of our staff, partners and beneficiaries and in benefit of life-saving aid.


